AMR in Orthopedics – Benefits of topical treatment and latest advances
In recent years, there has been a dramatic increase in the emergence of antibiotic-resistant bacterial strains making infection control increasingly challenging and limiting the choice of antibiotics available for treatment. A study from 2019 estimated that more than 2.8 million patients in the United States developed an antibiotic-resistant infection, leading to more than 35,000 deaths, with an associated economic burden of $55-70 billion dollars (Dadgostar 2019; Bhandari & Silburt 2021). It is believed that the frequent prescription of antibiotics across medical specialties with a known high risk of infection such as orthopaedics may be a contributing factor to the global increase of antibiotic resistance.
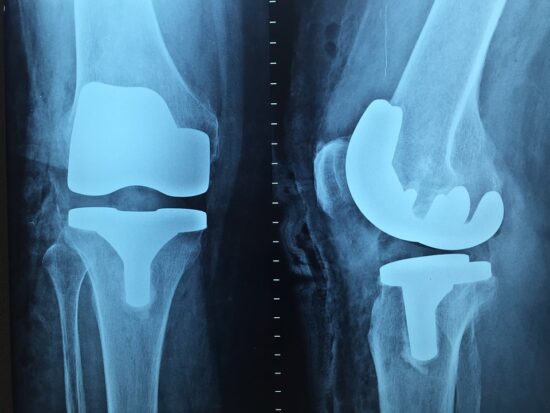
Periprosthetic joint infection (PJI) is a devastating complication of joint replacement surgery, associated with increased patient morbidity and a requirement for complex interdisciplinary management strategies (Aggarwal et al., 2013; Tande et al., 2014). Part of the difficulty in the management of this disease is that the bacteria associated with PJI can form bacterial biofilms. These biofilms are described as communities of microorganisms encased in a polysaccharide matrix. Upon attachment to a surface, biofilms display a high tolerance to antibiotics, compared to their planktonic counterparts which is believed to be one key means of antibiotic resistance in orthopaedic implant-associated infections (Stoodley et al., 2020). More recently, antibiotic resistant bacteria such as vancomycin-resistant enterococci (VRE) and carbapenem-resistant enterococci (CRE) have been reported in PJI infection and are linked to poorer outcomes (Kheir et al., 2017; De Sanctis et al., 2014).
Photo: credit IMGUR
AMR NEWS
Your Biweekly Source for Global AMR Insights!
Stay informed with the essential newsletter that brings together all the latest One Health news on antimicrobial resistance. Delivered straight to your inbox every two weeks, AMR NEWS provides a curated selection of international insights, key publications, and the latest updates in the fight against AMR.
Don’t miss out on staying ahead in the global AMR movement—subscribe now!